
Ekol Hospital's
Procedures

An unnoticeable, transparent – natural lens is placed just behind the coloured part of the eye. This lens is very transparent so that we see the pupil in the colour of black. This lens reflects the lights which is received by the eye on a layer of nerves and it must be definitely transparent so that the light can reach nerves. Anyhow, if this lens loses its transparency and gets blurred, this is called Cataract. This opacity can occur in any part of the lens or all around it.

The vision defects are corrected by Computer Automated Laser devices by changing the shape of the cornea. We can call this procedure shortly as “Laser Operation”. Excimer laser is applied to the corneal tissue which is at the front part of the eye and the carbon binds are broken; vaporizing the tissue and correcting the eye-sight. Cornea is “rasped” with the correct amount of laser waves directed to the desired area so the refractivity is changed and the desired values are reached.
- Myopia:- The corneal surface is probably very curved or the eye is longer than usual. The image is reflected in front of the retinal layer so the patient cannot see the far
- Hypermetropia:- The image is reflected behind the retina because the cornea is straighter or the eye is shorter than normal. The patient more likely cannot see the close.
- Presbyopia:- Elasticity of the ocular lens is decreased age relatively and the patients over 45 years old more likely have problems to see the close. By the result of natural aging the patients use reading glasses for the close sight and a second additional glass for the far.
PRK:- It’s the first application method of the Excimer Laser. The thin- alive layer over the cornea called “epithelia” is scratched by the “spatule” and excimer laser is applied right after the corneal surface is epithelia free within a 9 mm Radius.
TPRK:- This method is only applied with the Schwind Amaris Excimer Laser and the epithelia is not removed. The laser is applied directly on the cornea. The healing process is faster with this method.
Lasik:- It is a special procedure developed for more satisfying results with a minimum pain level. This procedure has 4 main advantages:
- Less pain than TPRK and the post-operative complaints disappear or gets minimum after the 2. day.
- The vision is corrected faster. The patient sees totally clear in 3-5 days.
- The eye numbers don’t increase again, the cornea doesn’t get blurry.
- Can be applied on myopia patients with the eye number up to 10.

Glaucoma starts mostly after the 40s without any symptoms and increases the eye tension. It is especially a condition of the optical nerves which transacts the images from the eye to the brain. Optical nerves are combined forms of the multiple nerve tendons. If those nerval tendons are damaged somehow, blind spots in the visual field might occur. Those blind spots mostly cannot be early diagnosed and when the nerval tendon is too much damaged; it’s too late which might lead to total blindness. Early diagnose of the glaucoma is very important in order to prevent any nerval tendon damages and blindness.
Laser treatment can be recommended for various types of Glaucoma. The microscopic channel system can directly be treated by laser in the open angle glaucoma. Laser is used to control the intra-ocular pressure by creating changes in the channel system (Trabeculoplasty). By the closed angle glaucoma, the laser is used to open a hole on Iris (Iridotomy) so that the drainage of aqueous humor liquid can be corrected.
A new channel is created by the surgeon using very thin & unique surgical equipments so that the aqueous humor liquid can be ejaculated from the eye (trabeculectomy). A surgical intervention might be recommended by your ophthalmologist in order to prevent further damage to the optical nerves. Like laser treatment; the surgical interventions also don’t need hospitalization.
Glaucoma treatment is a teamwork with the patient and the doctor. The doctor might recommend a treatment however, it is the patient’s duty to apply and stick to the instructions. When you start the treatment for the glaucoma, your ophthalmologist will call you more often for follow up controls. You should be ready to have control appointments every 3 or 4 months. This might be changed due to the course of your treatment. These regular controls & follow-ups will prevent any potential impairment risks.
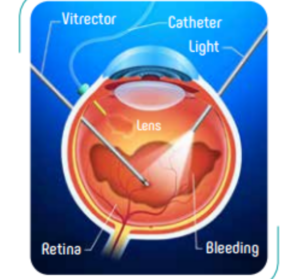
Eye related diseases can be split in two subject. The front part of the eye and the back. At the front, there is the cornea and the lens, and the Vitreous and Retina at the posterior part. The front part of the eye transmits the image to the posterior part. However, the posterior part completes the “seeing” by transmitting everything to the brain. Vitrectomy, also known as Pars Plana Vitrectomy surgery is the name of the surgery which performs holes smaller than 1mm on the retina and the gel at the posterior part
Vitrectomy application has many causes. This procedure is performed almost in every vitreous – related conditions. Most significant reasons for Vitrectomy are: Diabetic Retinopaty (Advanced pathologies in diabetes patients), Vitreous Bleeding (Intra ocular bleeding), Macular Pucker, Retinal detachment and tears ( ruptures of nerval system of the eye), macular holes, removal of a foreign object (post traumatic), post cataract operations (lens complications in), intra ocular infections after cataract or other eye surgeries.
It might be performed both under general anesthesia or local. Vitreous chamber and retina are reached via 3 holes of 0.5 mm created on the eye wall. After the intra ocular gel (vitreous) is cleaned via a probe which performs 1500 – 6000 incisions per minute, interventions are performed in order to correct the problems on the retina.

The structure of the veins is degenerated and bubbles occur, lead to bleedings and leakage of the fluid from the veins to the surrounding tissues. On the later stages, new buds occur on the retina and leads to sudden intraocular bleeding. The visual impairment develops at the later stages of diabetic retinopathy. Because of that a diabetes patient who doesn’t have any problem with the vision also should have regular examinations. Both eyes are mostly gets affected by diabetes and might lead to blindness.
Especially in the early stages, there is no need for a treatment if there is no macular edema. Blood sugar, blood pressure and colestrole should be under control in order to prevent diabetic retinopathy progress. Laser treatment should be applied to the whole retina in the case of proliferative diabetic retinopathy. This treatment is mostly 2 or 3 sessions. This treatment should be started before any intra ocular bleedings. It is unfortunately not possible to perform this treatment in the presence of strong bleeding. Vitrectomy operation is suggested if the bleeding is very dense. Blood is completely cleaned with vitrectomy and laser is performed.
Diabetic macular edema is treated by laser. Mostly, one session is enough however in some occasions the treatment might be repeated. If there is macular edema in both eyes one should be treated a few weeks after another. Generally, diabetes related risk of visual impairment is prevented %90 percent with laser. However, the laser can not help for the improvement of vision loss. Because of that, early diagnoses and treatment is important. Nowadays there are also alternative treatments to laser for the diabetes related macular edema. Anti – VEGF medicines might help treating the macular edema by preventing the formation of new unhealthy veins and preventing the leakages which leads to macular edema. These medications, which are injected in the eye can be used together with the laser or alone and might improve the vision. But it should be kept in mind that Anti – VEGF treatment is a surgical intervention and an injection inside the eye. So there are the risks of infection, retinal tears. It should be performed in a sterile operating theatre by experienced surgeons.
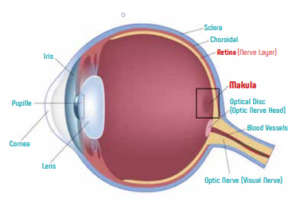
Retinal layer of the eye consists of nerve cells which transmits the light coming from outside to the brain. If the eye is like a camera, retina is the film. Macular area is just in the middle of this section. In the middle of the macula, there is the Foveo which is at the size of a pinhead where the light focuses. Foveo, also known as the yellow spot, gives the retina layer the abilities of central vision and detailed vision. Macular hole is the tear which appears right in the middle of the center of vision. A black dot appears in the vision of the patient which affects it badly. Recognizing the faces, reading newspapers or such activities are highly affected because of this condition. Since the other parts of the retina are normal, environmental vision is not affected. The most common reason of the macular hole is called “idiopatic” which is not related to anything and happens by itself. Age is somehow related to it. Other than that, traumas on the eye might also lead to macular hole.
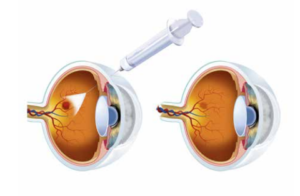
Even the factors which lead to macular hole are not exactly know, it is clear that the changes on the eye are mostly related to age. The intra ocular fluid, called Vitreous, shrinks by time, applies a pull force to the centre of sight and this force creates a hole on this area. Treatment of macular hole with medicine is not possible, the only treatment can be done is vitrectomy surgery. The vitreous fluid is cleaned, the membranes are pealed and a gas is injected into the eye. The vision might be lower after the surgery because of the gas inside the eye and the vision is corrected when the intraocular fluid replaces the gas by itself. The success rate of the operation, which means closing the macular hole is %80-90. However the rate is lower after the trauma or long-term holes. Macular hole surgery can be performed under local or general anesthesia. It is recommended to sleep on tummy for a while after the surgery to be sure that the hole is completely closed.
Retinal layer of the eye consists of nerve cells which transmits the light coming from outside to the brain. If the eye is like a camera, retina is the film. Macular area is just in the middle of this section. In the middle of the macula, there is the foveo which is at the size of a pinhead where the light focuses. Foveo, also known as the yellow spot, gives the retina layer the abilities of central vision and detailed vision. Distortion of the shapes and vision defect is mostly observed in the patients. Yellow Spot / Fovea is the most important part of the function of seeing. Eventough the retinal layer contain some veins, it also nourishes from the other rich veins which are located just beneath it.
The transition from dry type de wet type yellow type is an urgent condition. Thanks to the technologic improvements and modern treatment methods, the success rates of the treatment nowadays are very high. The aim of the treatment of the wet type yellow spot disease is to dry the leakages, bleedings and undesirable vein buds which are formed between the layers. There are alternative treatment methods
It is the oldest treatment method of the wet type yellow spot disease. The treatable occasions with this method are limited. Only %15 of the wet type yellow spot diseases can be treated standard laser method. Undesirable vein buds might relapse in %50 of the patients which are treated by laser
It’s developed after the standard laser treatment and it’s being applied since 10 years. A material called Verteporfin (Visudyn) is injected intraveneously and it’s binded to the damaged tissue in the eye. After that a laser treatment of 83 seconds is applied. It is beneficial in some types of wet type yellow spot disease. It doesn’t increase the vision however keeps the vision %50-60 within the 1 year treatment period. It’s rarely used as a solo treatment method in the suitable cases. Other than that, it is used combined with the injectible medications.
It’s the latest developed and most popular treatment method for the wet type yellow spot disease. It consists of Bevacizumab (Avastin, Altuzan), Ranibizumab alike active substances. Undesirable vein buds form between the layers at the posterior eye wall in the wet type yellow spot disease. This treatment prevents the formation of those vein buds and neutralizes the growth factors; stops bleedings and leakages. This treatment is repeated monthly and directly injected in the eye. Success rate of the protection of the vision is over %90 in 1 year period. Success rate of the improvement of the vision is around %30.
We Can Help You
We offer:-
-English speaking consultation
-Face to face, zoom or alternative calls with the appointed surgeon
-24/7 Assistance and care during your stay
-Advice and assistance on aftercare
-We can arrange flight and accommodation




